Smart Prioritization to Reduce Alarm Fatigue and Improve Response Times
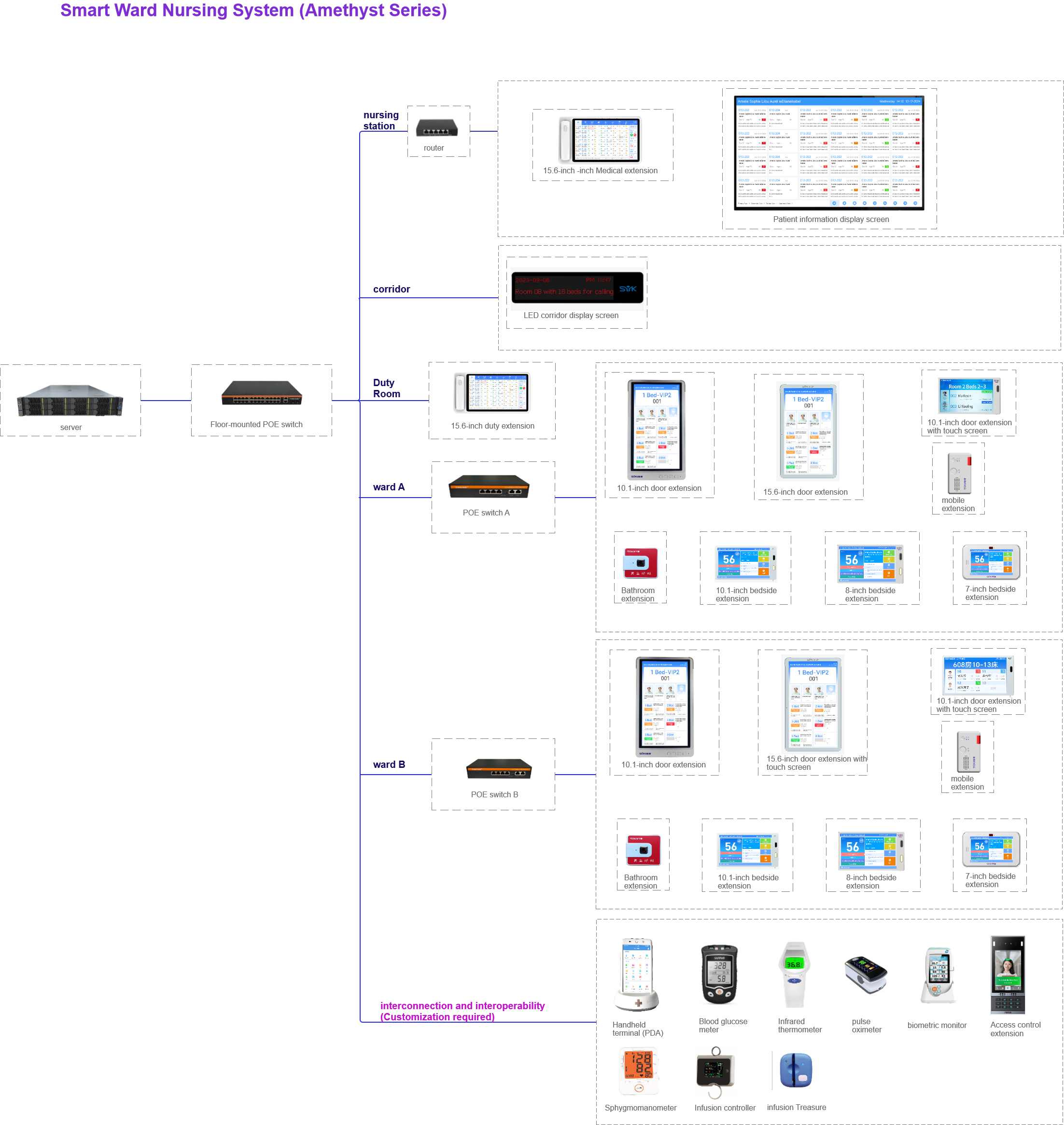
Clinical urgency triage using AI-driven severity scoring
Alarm fatigue continues to plague healthcare settings, where nurses often get overwhelmed by dozens if not hundreds of daily alerts that sometimes mask real emergencies. New nurse call systems are tackling this problem using artificial intelligence to score alert severity. These systems look at things like unstable vital signs, fall risk assessments, and past patient records to decide which calls need immediate attention. The smart sorting helps separate regular requests for help moving around from serious situations like heart issues, so only the most urgent cases reach nurses directly. According to recent data from the 2024 Nursing Efficiency Study, hospitals adopting these systems have seen around a third fewer false alarms. That means nurses spend less time chasing down non-emergencies and more time responding to actual medical crises. What's interesting is how these AI tools keep getting better over time as they learn from how staff actually responds to different types of alerts, helping prevent the numbness that comes from constant noise while speeding up responses when lives are truly at stake.
Real-time alert escalation paths for critical nurse call events
High severity alerts trigger automated escalation right away when something serious happens, like when oxygen levels drop fast or someone has a seizure. The system starts sending out alerts if the main nurse hasn't responded within about 45 seconds. First it goes to charge nurses, then moves on to rapid response teams, and eventually reaches whoever is nearby through their mobile devices thanks to location tracking features. This whole process works alongside real time staff management tools that know when people are taking breaks, switching shifts, or rotating between different units. A hospital group in one region saw their response times for cardiac arrests get better by 22 seconds after putting this system in place according to their 2023 quality report. Getting rid of all those manual steps means fewer mistakes happen because nothing slips through the cracks anymore. Plus hospitals stay compliant with those Joint Commission guidelines about managing alarms properly without even thinking about it.
Seamless Two-Way Communication and Mobile-Enabled Care Coordination
In healthcare settings, fast and secure ways to communicate are absolutely necessary for proper patient coordination. Mobile apps that keep things secure let clinical staff respond to nurse calls right from their phones or tablets using built-in voice and video features. This means they don't have to rely on those old physical stations anymore, plus everything stays encrypted according to HIPAA standards all the way through. When nurses can actually see what's going on with patients before walking into their rooms, it makes a huge difference. This visual check is especially important when dealing with contagious diseases or situations involving behavioral health issues where quick assessment matters most.
Integrated voice/video nurse call response via secure mobile apps
Staff can accept or escalate calls with one tap while accessing EHR data through unified interfaces. Real-time translation capabilities break language barriers during emergencies, and encrypted screen-sharing supports rapid clinical consultations. Devices with hands-free operation enable communication during sterile procedures, reducing response latency by 72% (2024 Clinical Workflow Study).
Dynamic staff assignment and location-aware notifications
Smart systems send alerts straight to the closest available caregiver thanks to real time location tracking tech. If someone presses their emergency nurse button, the system looks for staff who are actually certified to handle it within about 15 meters away. Then it checks what shifts those nurses are on right now plus which patients they're already assigned to before sending out priority messages directly to their phones down to specific rooms. The results? Hospitals report missing only about 32% of calls compared to before, and most responses happen faster than 45 seconds according to recent studies from Healthcare Mobility Research back in 2023.
EHR Integration and Automated Documentation for Regulatory Compliance
Modern healthcare facilities require seamless data flow between critical systems. Integrating nurse call platforms with Electronic Health Records (EHR) creates a unified clinical ecosystem—ensuring contextual patient data is instantly available during emergencies while automating regulatory workflows.
Bidirectional nurse call–EHR synchronization for contextual clinical data
Two way syncing helps get rid of those annoying data silos that happen when different systems don't talk to each other properly. When someone makes a call, important patient details pop up right on their screen. Things like what meds they're taking, if they're at risk of falling, and what treatments are planned all show up automatically for responders to see. At the same time, whatever gets done during the actual response, whether it's checking pain levels or treating wounds, gets added straight into the medical record without anyone having to type it in later. The whole process cuts down on how long staff spend documenting stuff by around half, which means nurses and doctors can actually spend more time taking care of patients instead of filling out forms between shifts.
Auto-generated audit trails and CMS-compliant documentation
The automated systems create detailed audit trails that can't be altered, which meets all those CMS requirements healthcare facilities have to follow. When something happens during a call, the system automatically logs everything important like when it happened, who responded, and how they fixed whatever problem there was. No need for anyone to type this information in manually anymore. These systems come with customizable forms that fill themselves out for things like patient checkups, treatment notes, and all those reports about quality metrics that administrators love so much. Mistakes in medical records basically disappear with this setup, and hospitals stay ready for audits at any time. According to a study from Healthcare IT in 2023, these systems cut down on compliance issues by around two thirds. Plus, clinics save about 15 hours each week that nurses would otherwise spend on paperwork, letting them actually spend more time taking care of patients face to face instead of staring at computer screens.
Enterprise-Grade Reliability, Security, and Scalability for Acute Care
In acute care settings, nurse call systems need to be built for situations where everything matters because when these systems fail, patients are at risk. The best enterprise level solutions tackle this problem by having backup systems ready to take over automatically if something goes wrong. These setups keep running almost all the time, even when there are problems with the internet connection or power cuts happen unexpectedly. When it comes to keeping information safe, these systems go beyond what's required in healthcare. They use strong encryption from start to finish, handle patient data according to HIPAA rules, and have monitoring systems that catch anyone trying to get into private communications without permission. Healthcare organizations that are expanding find that these systems grow right along with them. Whether they're just adding more beds to current wards or bringing whole new buildings online, the service quality stays the same. During busy times when hospitals are full, these systems continue performing reliably while protecting important medical records from hackers who constantly develop new ways to steal sensitive information.
FAQ
What causes alarm fatigue in healthcare settings?
Alarm fatigue results from nurses being overwhelmed by numerous daily alerts, which may sometimes desensitize them to actual emergencies.
How do AI systems improve response times?
AI systems prioritize alerts based on severity, ensuring urgent cases receive immediate attention and thereby improving response times.
Are nurse call systems secure?
Yes, modern nurse call systems ensure secure communications, adhering to HIPAA standards and using encryption.
How do location-aware notifications work?
These notifications use real-time location tracking to alert the nearest certified staff member to respond quickly to emergencies.